What is pain?
Pain is an individually perceived unpleasant sensory and emotional experience. It is a highly personal experience. Pain may alert us to harmful changes in the body,or immediate environment.
In other cases, pain exists or continues without any known cause or benefit. Pain that continues for longer than three months is called chronic pain. Chronic pain can happen without a known cause and persist after an injury or known cause is resolved. It can affect a person’s mood, relationships, movement, and all aspects of daily life. Pain can make it harder to do necessary tasks, work, and enjoy activities.
Patterns and types of pain
There are three primary patterns of pain, which are named based on how long the pain lasts and its frequency.
- Acute pain starts suddenly and ends when its cause is treated or healed. The feeling of acute pain is usually sharp because it tends to act as a warning signal about a threat to the body from an injury, disease, overuse, or other environmental stress. Common causes for acute pain are strained muscles, broken bones, dental work, surgery, childbirth, infections, and/or burns.
- Episodic pain happens from time to time and may be at irregular intervals. It may be associated with a long-term medical condition, like sickle cell disease. Painful periods and chronic migraine are examples of episodic pain. It can happen out of nowhere or may be caused by known triggers.
- Chronic pain lasts for longer than three months or the expected healing time. In some cases, an acute pain condition might persist and become chronic pain. In other cases, chronic pain happens for no known reason. People might experience one or more chronic pain conditions, or chronic and acute pain, at the same time.
Pain can also be put into categories based on its most likely source. In many cases, pain fits in to more than one of these categories:
- Nociceptive pain describes pain that is caused by tissue damage and/or inflammation. The sensation can be sharp, pricking, dull, or aching, depending on what caused the damage or inflammation. Examples of nociceptive pain are pain from a paper cut, an infection, a broken bone, or osteoarthritis.
- Neuropathic pain describes pain that is caused by nerve damage due to an injury or disease. Neuropathic pain sensations are often described as burning, tingling, shooting, or like electric shocks. Examples of conditions that cause neuropathic pain are diabetic neuropathy, shingles, and sciatica.
- Nociplastic pain describes pain that is caused by changes in how the nervous system processes pain. The changes that cause nociplastic pain are not linked with a clear injury, tissue damage, inflammation, or disease. The sensations related to this kind of pain vary widely. Examples of nociplastic pain include fibromyalgia, irritable bowel syndrome, and chronic low back pain.
What causes pain?
There is still much to learn about how and why people feel pain in different ways. Acute pain with an obvious cause (an infection or broken bone, for example) is much better understood than chronic pain. Research shows that factors and changes in the body (biological), the mind (psychological), and a person’s experiences with others along with the conditions in their environment (social) are all contributors to an individual’s experience of pain. For this reason, pain is known as a biopsychosocial experience.
Biological factors associated with pain include things like brain function and genetics. Psychological factors are things like mood and stress. Social factors include things like having (or not having) a support system or experiencing biased care. Each set of factors affects and impacts one another. Therefore, treatment for pain is both complex and individual.
Biological factors of pain
Many different biological factors are involved in the experience of pain, including the type of injury to the body, genetics and epigenetics, the nervous system, the immune system, and the endocrine system.
Genetics and epigenetics of pain
Each of us is born with a set of genes that we inherit from our parents. However, daily life stressors, lifestyle habits, and medical conditions influence which genes turn on or off over a person’s lifetime. This is the difference between genetics, or the study of genes and heredity, and epigenetics, or the study of how the environment and behaviors change how genes work.
Many genes play roles in how a person feels pain, their risk for developing chronic pain, and how well they respond to pain treatments. This risk comes from genes that control the function of body systems involved in pain and relief. It can also come from genes linked with medical conditions that cause pain. For example, some causes of back pain, such as ankylosing spondylitis (a form of arthritis that affects the spine), have a genetic component. Although genetics might put someone at risk, epigenetics can influence whether that risk becomes a reality.
Previous research, for example, has shown that epigenetic changes following regular physical activity are linked with positive changes in a person’s pain experience. Other research has shown that intense emotional stress can cause epigenetic changes in pain-related genes that lead to worse pain outcomes. Newer research is helping us understand how experiences of long-term stress due to social factors like neighborhood, access to healthy food and good medical care, and other social determinants of health contribute to consistent group differences (called disparities) in pain.
Pain and the nervous system
The human nervous system is made up of two main parts: the central nervous system and the peripheral nervous system.
The central nervous system includes the nerve cells that make up the brain and spinal cord. Brain systems involved in the experience of pain overlap with systems involved in the experience of emotions like fear, anxiety and anger, reward and motivation, attention and memory, and sensation. There are also brain systems that contribute to relief from pain. Research shows that changes in these brain systems might contribute to chronic pain risk.
The peripheral nervous system includes nerve cells that start in the spinal cord and extend out to other body parts. These nerve cells carry information between organs/muscles and the spinal cord, which links the information to the central nervous system.
Peripheral sensitization and central sensitization are terms to describe changes in the peripheral and central nervous systems that make a person more sensitive to pain and other sensations. These changes are one way some people develop chronic pain after an injury has resolved.
Symptoms of nervous system sensitization
Hyperalgesia happens when something that is already painful to a person begins to feel even more painful to that person. Allodynia is the term for when something that previously was not painful to a person begins to feel painful. For example, a person might experience allodynia when light touches feel painful on sunburned skin. Global sensory hyperresponsiveness means the person is very sensitive to many or all sensations, including lights, noises, smells, and foods.
Pain and the immune system
The immune system helps protect the body from outside invaders, like bacteria and viruses, to avoid potential infection. One way the immune system provides protection is through inflammation. Inflammation is a reaction that happens when tissues are injured and damaged cells release chemicals that cause swelling and attract immune cells to “eat” the dead or damaged cells. This process helps with healing.
In some cases, the immune system is overprotective, and inflammation lasts longer than the expected healing time. This overprotection can backfire and contribute to more and longer lasting pain. Another way that the immune system can be overprotective is called autoimmunity, which happens when the body’s immune system attacks healthy cells. Some autoimmune conditions cause chronic inflammation and pain.
The endocrine system
The endocrine system is responsible for making hormones, which are a type of chemical messenger that carries instructions throughout the body. Stress-related hormones like cortisol and adrenaline can send messages that make the feeling of pain more intense or less intense. This is partly why finding helpful ways of coping with stress can help lower pain intensity. Additionally, research shows that chronic pain may lead to changes in the way the endocrine system functions over time.
Psychological factors that contribute to pain
Fear and avoidance
Imagine this scenario: Jason injured his back while lifting a box at work. His healthcare provider tells him not to lift heavy things for a few months to heal. But after Jason’s back feels better and he is cleared to return to regular activities, he is still worried about re-injuring his back. This is an understandable fear. But this avoidanceof lifting things has been affecting Jason’s work and home life. He also avoids doing his physical therapy exercises, making his muscles weaker over time. His mood and stress levels are also affected.
This scenario is an example of the fear-avoidance model of pain. Although fear and avoidance can help protect a person from dangerous situations, they can also hinder recovery from acute pain and play a role in the transition to chronic pain. Avoidance also contributes to disability and often stops a person from doing the things they enjoyed before the pain started, which can affect a person’s mental health.
Emotions, mood, and mental health
It is common for pain, especially chronic pain, to affect a person’s emotions and mood. For example, many people with chronic pain describe times when they feel anger, worry, sadness, guilt, grief, defeat, hopelessness, frustration, depression, or anxiety because of their pain.
While pain can influence a person’s mood, emotions, and mental health, those factors can also influence a person’s experience of pain. This exchange happens partly because the brain systems involved in emotions, mood, some mental health conditions, and pain overlap. Research shows that major depression, generalized anxiety disorder, post-traumatic stress disorder (PTSD), and sleep problems commonly co-occur with chronic pain. Getting necessary support to help manage the emotions, moods, and mental health conditions that co-occur with pain has been shown to improve chronic pain symptoms, such as muscle tension.
Resilience
Resilience reflects a person’s ability to bounce back from and adapt to life’s challenges, such as living with chronic pain. Being resilient does not mean a person is free from worries, anxiety, sadness, anger, or grief about their pain. These emotions are normal and understandable responses to the experience of living with pain. Instead, being resilient means using personal strengths to adapt to the challenges of pain. Examples are a person’s social supports and community, ability to solve problems, humor, use of coping strategies (e.g., deep breathing, prayer), and activities that bring more joy to their life.
Resilience is not something a person is born with or without. Resilience is easier on some days than others and can be built and strengthened with support and practice.
Beliefs and thoughts about pain
Research shows that beliefs and thoughts about pain also affect a person’s experience of pain. There are some common thinking styles that co-occur with chronic pain. They often happen so naturally that they are called “automatic” thoughts.
- Ongoing concerns about pain: There are many of unknowns when living with chronic pain. Will it ever go away? Will it get worse? These kinds of normal concerns can lead to hopelessness, anxiety, and depression when they continue for a long time.
- “Should” statements: Pain can change the way a person lives their life, causing them to reduce or even stop some activities. Sometimes, a person might feel pressure to live life in the same way they did before. One might experience thoughts that could cause feelings of frustration, anger, and disappointment when expectations don’t align with reality (for example, “I should still be able to do this perfectly,” or “My pain should get better right away.”).
- Self-blame: If chronic pain starts after an accident or a medical condition, a person might blame themselves for the pain being triggered (for example, “If only I hadn’t driven to work that morning,”). But, predicting an accident or the onset of a medical condition is often outside of a person’s control.
These beliefs and thinking styles don’t just come out of thin air. They come from a person’s previous experiences and can be a normal reaction to difficult circumstances. However, they can lead to negative emotions and increase pain symptoms. Getting necessary support to figure out which pain beliefs are helpful, and which might not currently apply or might get in the way of recovery, has been shown to improve chronic pain symptoms.
Social factors that contribute to pain
The social determinants of health include the quality of the environments where people are born, live, learn, work, play, worship, and grow older that affect health outcomes. They also include the wider set of policies and systems that shape the conditions of daily life. Some examples of social determinants of health include economic stability, access to quality education and healthcare, living in neighborhoods with safe places to walk, and having close relationships.
Compared to our understanding of the biological and psychological factors involved in the experience of pain, less is known about the role of the social determinants of health. New research in this area is ongoing and will help address disparities in pain and pain care.

STRUCTURE
Introduction
Step 1
Step 2
Step 3
Step 4
Is part of a series . .
Gentling Yourself to be the pinnacle.
Here biology and when not living acc to the blueprint – we get told. PAIN
PAIN – 3 messages
PAIN – WHY THERE- WHAT SET IT UP (why you not the next person) and WHAT IS TO BE LEARNED?
1 – When calmer, does not hurt so much
2 – Pain anywhere is because of STUCK – anywhere
3 – Nutrients and circulation not perfect.
ME – and how I got to be here 5.15
Historical – women finding me – undoing upset. . .
Bach flowers . . .and undo emotional state – labour easier
Women’s lives hurt . .
How we feel dictates what goes on in our body . .
EXPERIENCE matters – so what you find here may not be elsewhere .
BEING WOMAN SHOULD NOT HURT 3.43
Biology – let us look to what is in store . ..
And thus – how could we be alive if we were in pain all the time?
RESOURCES – heatherbrucehealing.com/welcome-to-your-lady-bits/ Structure Determines Function
TO DO
What are you doing to make things better?
What do you think listening so far that you may have done to contribute to continuing being in pain?
1 – START – WHAT IS YOUR GOAL? 2.51
Surprising package – have to change . .
See here this goes – pain is a great motivator – want to know what life would be like – without it.
TO DO
What is your goal? (Out of pain?)
2 – INTRO/Goals 4.31
hello –
RESOURCES
SHEN info
Pain – from WDCD
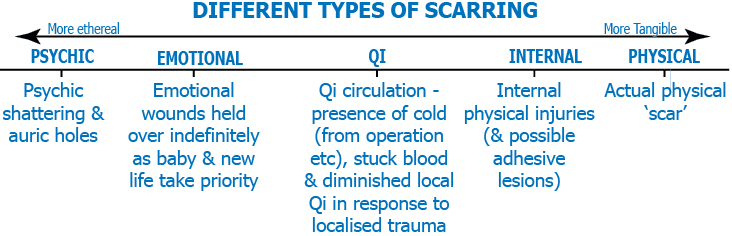
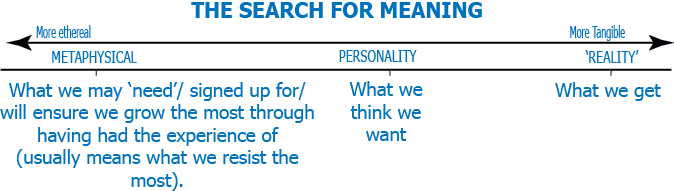



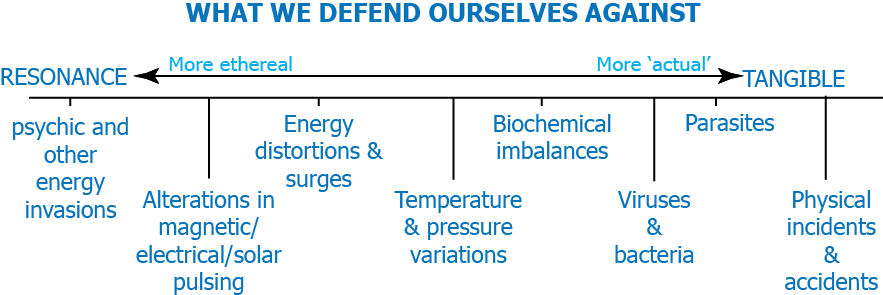
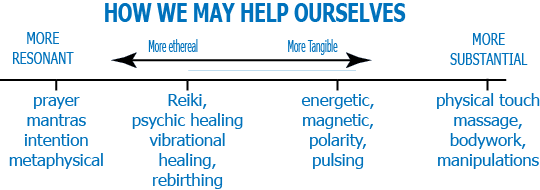

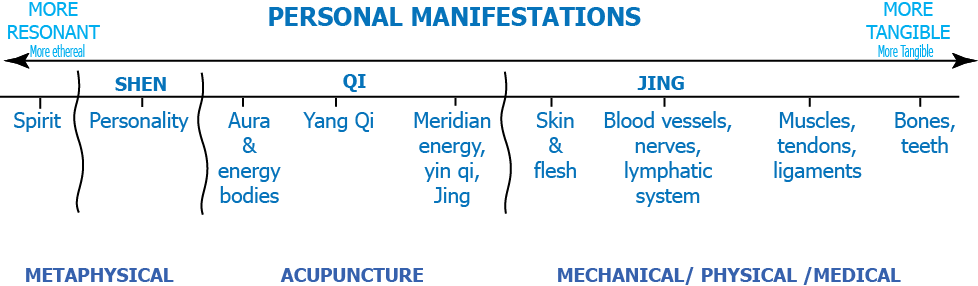
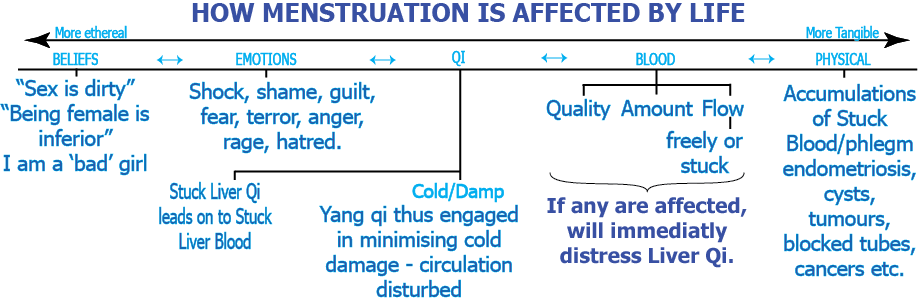
More upset – more it will hurt
Pain is a message – (Prove me wrong)
Pen and paper – water, how could I do this better?
As if I was the most important person in my life”
When did pain start? What body needs? Change – what you do dictates what happens
YOU – feel the changes IF you change .
Tribal natter – introducing yourself.
TO DO
Pic, where you live, your pain -where and when. so you have a bunch who are also sharing your journey .
When did pain start? What body needs
WHY IT HURTS?
WOMB NOT IN RIGHT PLACE
https://heatherbrucehealing.com/womb-work-centering-a-womansbody/
ANSWERING PART OF WHY A PERIOD HURTS . ..
PAIN IS TEMPORARY 2.54 – before action
Magnesium
iodine – breasts, reproduction, cell life and death, clear brains and energy easily
Pain is not a given .. .undo breakage
SEASONS OF A LIFE 3.42
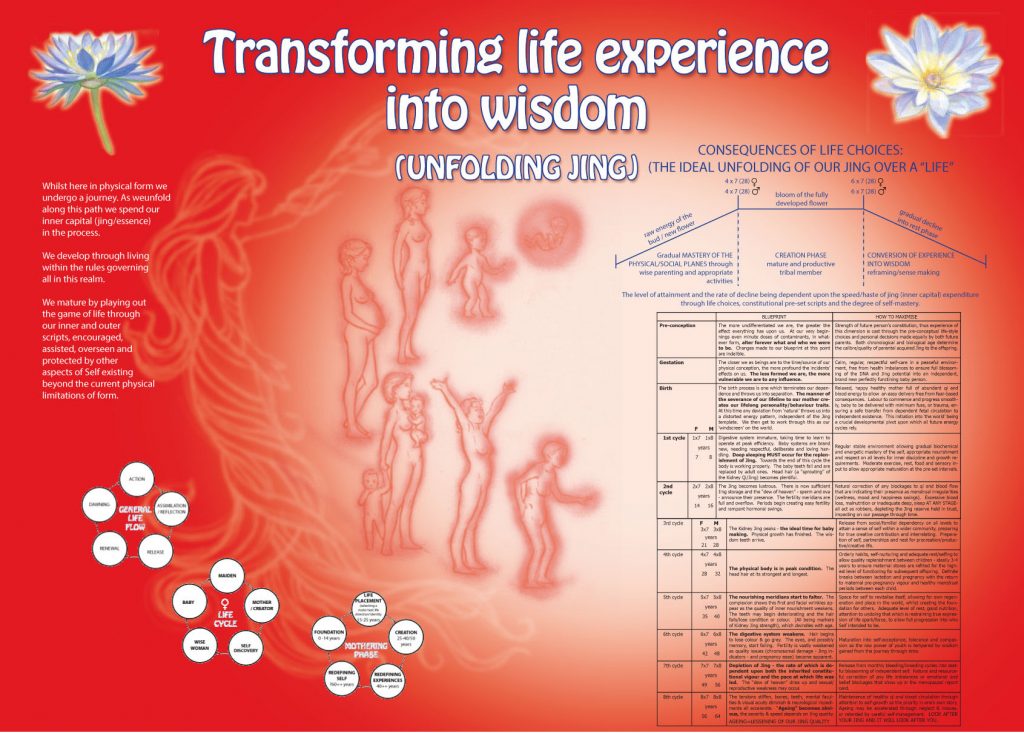
Sun – sleep
Moon – periods
Year – seasons
Life – Jing
